Oct 04, 2017 by

29 per cent of adult Americans suffer from lower back pain (Belluz, 2017). Lower back pain is one of the most common reasons to seek medical aid and is the leading cause of job disability in the world (American College of Physicians, 2017; MacMillan, 2017). It can become chronic if it is not treated in a timely manner (Belluz, 2017). There are a variety of treatments for lower back pain such as prescription drugs, exercise, massage therapy, acupuncture, and more. However, each treatment is not completely effective on its own, and often combines a variety of treatments in conjunction to help lessen the pain and improve lower back pain health. In fact, the American College of Physicians (ACP) recommends spinal manipulation, acupuncture, heat, and massage therapy for lower back pain before using drug therapy because drugs are riskier than alternative treatment options (American College of Physicians, 2017).
There are different categories of pain: acute (lasting less than four weeks), subacute (lasting four to 12 weeks), and chronic (lasting more than 12 weeks) (American College of Physicians, 2017). Acute lower back pain tends to come from the inflammation as a result of torn muscles or strain (Ullrich). About 85 per cent of people with back pain suffer from “nonspecific low back pain” – pain that has unknown causes – which makes chronic nonspecific low back pain a pain to treat (Belluz, 2017). However, since alternative treatments help treat lower back pain, these can also be used as part of prevention and improving your back health.
Popular treatments in the past for this problem (now proven to be ineffective and can be harmful) included bed rest, spinal surgery, opioid painkillers, steroid injections (Belluz, 2017). As the ACP pushes physicians to prescribe alternative methods, studies are conducted to determine if they really help. Here is a list of therapies for lower back pain:
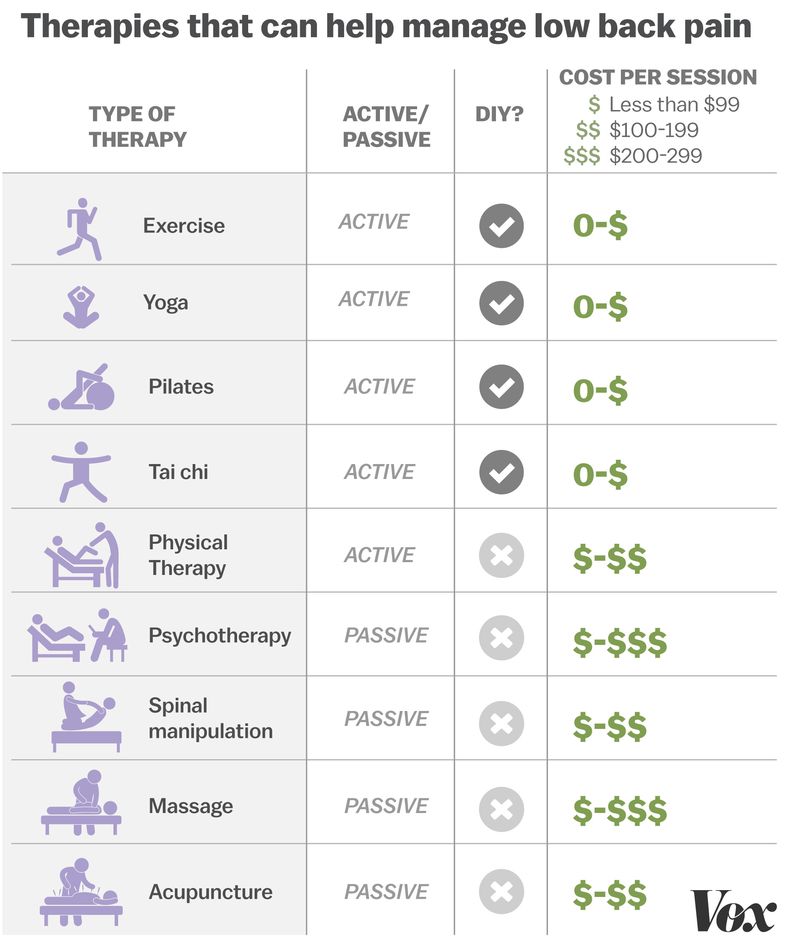
A study showed that after 10 weeks of massage therapy, over a third of patients said their pain was nearly or completely gone compared to other patients who did not receive massage therapy (Goodman, 2011; Real Bodywork, 2017). The researchers from this study measured variables of pain, quality of life, and physical functionality/disability; and the improvements for each are significant (Real Bodywork, 2017). It is not a surprise when patients feel improvements from massage therapy since massages have been traditionally beneficial (Real Bodywork, 2017).
“For the treatment of chronic low back pain, physicians should select therapies that have the fewest harms and costs, since there were no clear comparative advantages for most treatments compared to one another”, says Nitin S. Damle, MD, MS, MACP, and president of ACP. Opioid prescriptions are common for people with back pain – 20 per cent of these prescriptions are long-term (Belluz, 2017). With opioids, there is a risk for addiction and It is estimated that more than 30,000 Americans will die from opioid overdoses in 2017 (American College of Physicians, 2017; Belluz, 2017).
Biopsychosocial is the act of taking into account of one’s physical, psychological, and social factors that play a role in the experience and reduction of pain (RMT Education Project). Biological factors include physiology; psychological factors include thoughts, emotions, and behaviors; and social factors include culture and religion (RMT Education Project). For example, those who have stress, depression, anxiety, or a history of trauma tend to suffer more (Belluz, 2017). There is an emerging understanding of pain called “central sensitization” – which means that one’s pain sensitivity is heightened due to malfunctioning pain signals (Belluz, 2017).
Massage therapy is the manipulation of soft-tissue, usually performed by trained therapists (Dahmer, 2010). Massages “can help relieve muscle tension, reduce stress, and evoke feelings of calmness”, thereby increasing the production of “feel good” chemicals called endorphins, and help improve sleep quality (Dahmer, 2010; Ullrich). It can also prompt positive psychological effects that may contribute to tissue repair and pain modulation (Dahmer, 2010).
Researchers from McMaster University in Canada found that massage causes the activities of genes to change in a way that reduces inflammation in muscles – similar to when you take an aspirin or ibuprofen (Szalavitz, 2012). As well, massage sets off a chain of molecular events in muscles that helps reverse the discomfort from exercise (Szalavitz, 2012). Blood flow and circulation is increased during a massage, which helps bring nutrition and oxygen to muscles, and metabolic waste away (RMT Education Project; Ullrich). As a result, patients of massage therapy was able to recover from exercise and injury quicker (Szalavitz, 2012; Ullrich).
If getting a massage from a therapist is inconvenient – whether it may be due to time constraints, cost restrictions, or preferences of personal privacy – consider giving yourself a massage with a hand-held massager (Rodts; Ullrich). Hand-held massagers are a good investment because it provides convenience and is cost-effective.
Massage therapy may be particularly effective when combined with exercise and education, concluded the Cochrane Review (Dahmer, 2010). Since exercise – like massages – increases blood flow, physical activity can help relieve pain (Belluz, 2017). As a result, being inactive to “recover” can delay one’s recovery – which is contrary to popular belief (Belluz, 2017). Like massage therapy, exercise needs to be done long-term as part of one’s lifestyle (Goodman, 2011).
Physical activity can also increase the “feel good” chemicals in the body too; especially when someone finds something they enjoy doing (Belluz, 2017). When this happens, patients gain confidence over the problem and make it manageable for the rest of their life (Goodman, 2011). Indeed it may be difficult to break the pain-inactivity cycle when it hurts to move, but starting slow will help you gain traction for treatment (Goodman, 2011).
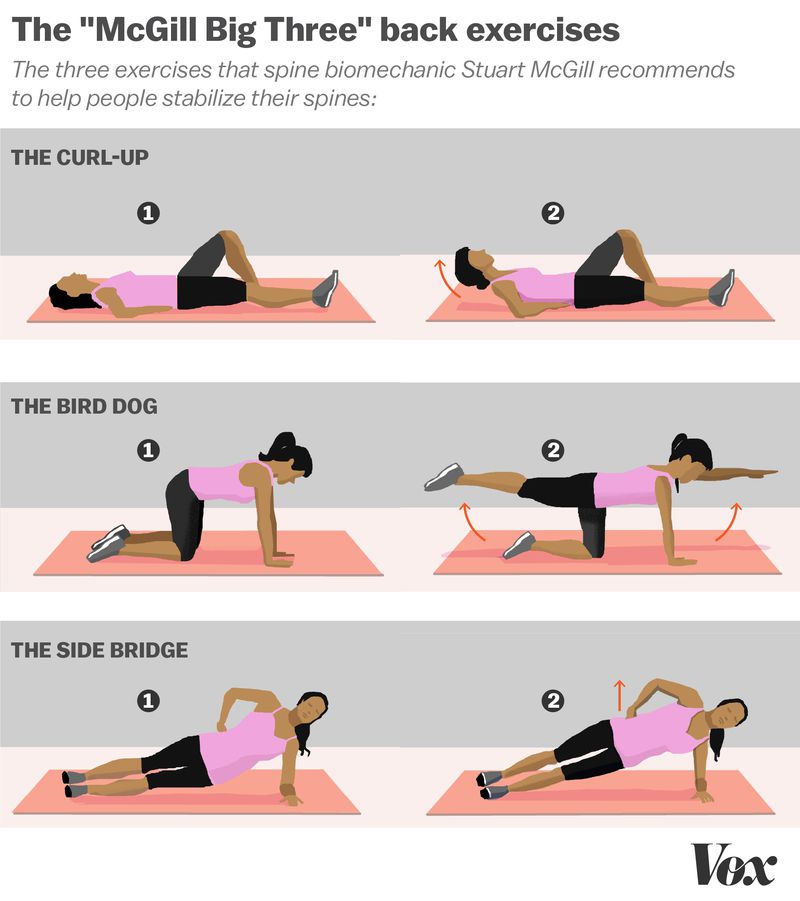
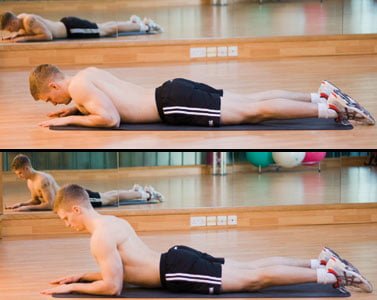

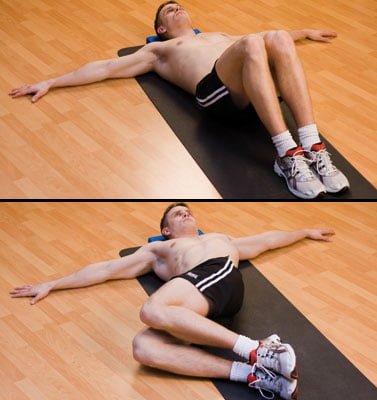
PNF stands for Proprioceptive Neuromuscular Facilitation, which is an advanced form of flexibility training that incorporates both stretching and contraction of the targeted muscle group (Walker, 2017). This type of stretching was developed for rehabilitation, but it is also found to be effective for increasing flexibility and muscle strength because it relies on reflexes that produce deeper stretches (Barta, 2017; Walker, 2017).
PNF stretching works best with muscles along the “long kinetic chains” in the body, which includes the side fascia, hip flexors, hamstrings, glutes, and back – all related muscles that cause lower back pain (Barta, 2017). The individual contracts the muscle during the stretch while their muscles are movement-restricted (Walker, 2017). The length of contraction and number of repetitions depends on the individual.
In some areas of the world, health insurance makes alternative treatments difficult to obtain (Belluz, 2017). For example, it is easier for someone to get opioids and back surgeries than a massage or exercise program reimbursed (Belluz, 2017). This is reactive treatment, not proactive prevention. However, since alternative treatments have evidence of success, they can be used as part of prevention as well.
American College of Physicians issues guideline for treating nonradicular low back pain. (2017, February 14). Retrieved September 22, 2017, from https://www.acponline.org/acp-newsroom/american-college-of-physicians-issues-guideline-for-treating-nonradicular-low-back-pain
Barta, K. (2017, February 10). PNF Stretching: A How-To Guide. Retrieved September 25, 2017, from http://www.healthline.com/health/fitness-exercise/pnf-stretching#overview1
Belluz, J. (2017, August 04). A comprehensive guide to the new science of treating lower back pain. Retrieved September 22, 2017, from https://www.vox.com/science-and-health/2017/8/4/15929484/chronic-back-pain-treatment-mainstream-vs-alternative
Dahmer, S., Teets, R. Y., & Scott, E. (2010). Integrative Medicine Approach to Chronic Pain. Primary Care: Clinics in Office Practice, (37), 407-421. doi:10.1016
Exercises for lower back pain – Live Well. (2015, January 2). Retrieved September 25, 2017, from http://www.nhs.uk/Livewell/Backpain/Pages/low-back-pain-exercises.aspx
Goodman, B. (2011, July 05). Study: Massage Helps Treat Low Back Pain. Retrieved September 22, 2017, from http://www.webmd.com/back-pain/news/20110705/study-massage-helps-treat-low-back-pain
Kumar, S., Beaton, K., & Hughes, T. (2013). The effectiveness of massage therapy for the treatment of nonspecific low back pain: a systematic review of systematic reviews. International Journal of General Medicine, 733. doi:10.2147/ijgm.s50243
MacMillan, A. (2017, April 6). Massage Can Help Treat Lower Back Pain. Retrieved September 22, 2017, from http://time.com/4728672/massage-low-back-pain/
Massage Therapy and Back Pain. (n.d.). Retrieved September 22, 2017, from http://www.rmtedu.com/blog/massage-therapy-and-back-pain
“Real-World” Massage for Chronic Low Back Pain. (2017, April 10). Retrieved September 26, 2017, from http://www.realbodywork.com/real-world-massage-chronic-low-back-pain/
Rodts, M. (n.d.). Can Therapeutic Massage Help Relieve Back Pain? Retrieved September 22, 2017, from https://www.spineuniverse.com/treatments/alternative/can-therapeutic-massage-help-relieve-back-pain
Szalavitz, M. (2012, February 02). How Massage Helps Heal Muscles and Relieve Pain. Retrieved September 22, 2017, from http://healthland.time.com/2012/02/02/how-massage-helps-heal-muscles-and-relieve-pain/
Ullrich, P. (n.d.). Can Massage Help Your Back Problem? Retrieved September 22, 2017, from https://www.spine-health.com/wellness/massage-therapy/can-massage-help-your-back-problem
Walker, B. (2017, May 24). PNF Stretching Explained – Proprioceptive Neuromuscular Facilitation. Retrieved September 25, 2017, from http://stretchcoach.com/articles/pnf-stretching/